Gyan Burman Liver Surgery Unit, Sir Ganga Ram Hospital,
2222, First Floor, New Delhi-110 060, India
Gyan Burman Liver Surgery Unit (GBLSU) is an extension of Department of Surgical Gastroenterology which was created in 1997 to fulfill a long standing need to deal with complex gastrointestinal surgery in parallel with developments elsewhere. Surgical Gastroenterology was coming in to its own in various teaching hospitals all over India in the late eighties. The first to be established in North India was the Department of Gastrointestinal Surgery in All India Institute of Medical Sciences under Professor S. Nundy in 1985.
This department now has an outstanding reputation for all aspects of liver surgery. Complex liver resection can be carried with a mortality and morbidity comparable to the best centres in the world. There is also can an active interventional radiology setup that deals with chemoembolization, radio-frequency ablation and percutaneous alcohol injection into tumor tissue.
 This centre is very active in liver transplantation and is equipped for both cadaveric and living related transplant. It has to its credit first successful reduced liver transplant from an adult cadaveric liver to a pediatric recipient.
This centre is very active in liver transplantation and is equipped for both cadaveric and living related transplant. It has to its credit first successful reduced liver transplant from an adult cadaveric liver to a pediatric recipient.
Pancreatic surgery is also carried out in great numbers and possibly we have one of the largest series of pancreaticoduodenectomy operation for cancers of the periampullary region. The department has treated patients from all over India as well as patients from Middle East, Africa and South East Asia. Apart from malignancies this department has considerable skills in dealing with surgical management of all aspects of pancreatitis. Its faculty consists of nationally and internationally known consultants.
This department has a reputation for shunt surgery for patients who have bled from varices. In situations where the liver is not diseased, then shunt surgery is quite an appropriate form of treatment. Often because of blockage of hepatic veins mesocaval shunts can reverse the damage to liver.
This department is a referral centre for patients who have been operated elsewhere and has developed a complication. One such common condition is intestinal fistula and these have been managed very successfully here. A paper from our department was awarded the best paper in one of the recent Indian Society of Gastroenterology meetings. The department has a very active Stoma Clinic, which deals with wound care in intestinal fistulae.
Colorectal cancer is another active area of our department and there is a major emphasis on sphincter saving surgery either using staplers or by intersphincteric resection. Ulcerative colitis generally can be treated by medicine but surgery has a major role in certain situation. The entire diseased colon is removed and the end of small intestine folded on itself and joined to create a pouch, which is then joined to the anus so that the patient can pass stool normally.
The department has skilled consultants who are backed by a huge team of experienced registrars, theater personnel and equipment such as ultrasonic aspirator, argon beam coagulator and thromboelastograph which all helps in conducting major surgery.
The Department of Surgical Gastroenterology has a proven track record of dealing with complex gastrointestinal cases and is at the forefront of clinical medicine and liver surgery in India.
LIVER TRANSPLANTATION
Liver transplantation is the surgical replacement of a diseased liver with a healthy liver. The indication for this operation is end-stage liver disease, characterized by patients suffering from reduced liver function, muscle loss, fatigue, encephalopathy, signs of portal hypertension (see portal hypertension surgery), poor blood clotting and jaundice. A variety of liver diseases can lead to end-stage liver disease. There are generally two main categories: those cases caused by viruses (Hepatitis B and C) and/or alcohol and those caused by problems concerning the bile ducts (primary biliary cirrhosis and primary sclerosing cholangitis). There are other causes of end-stage liver disease, but they are less frequent. Prior to transplantation, a multidisciplinary liver transplant team evaluates potential liver recipients
After an evaluation is completed, the patient is placed on the liver transplant waiting list. In India ORBO (Organ Banking and Retrieval Organization) and MOHAN (Multi Organ Harvesting and Networking) promote organ donation and facilitate distribution of cadaveric livers.
There are different sources of donor livers. Usually the liver is obtained from a cadaveric donor (a person diagnosed as "brain dead" but whose other organs and systems are functioning properly). Due to a continuous shortage of donor livers and the high incidence of liver disease, the waiting time is increasing every year. Hundreds of people die each year while waiting for a cadaveric liver to be offered. Donor livers also can be obtained from a family member or a friend who donates a portion of his/her liver to the patient (see living-related donor).
In the case of a cadaveric donor organ, the transplant center receives a liver offer from ORBO for a specified patient. . The patient is then notified and admitted to the hospital. While the donor team is procuring the donor liver, the recipient team begins to prepare the patient. The diseased liver is removed and the healthy liver is put in its place. The operation usually takes 6-8 hours. After the operation the patient begins taking medications to prevent the new liver from being rejected by the body. Complete recovery may take several weeks. The quality of life for transplant patients usually improves dramatically and most lead healthy, normal lives.
LIVER SURGERY
Liver surgery comprises various operations of the liver for different disorders. The most common operation performed on the liver is a resection (removal of a portion of the liver). The most typical indication for liver resection is a malignant tumor. Tumors can be primary (developed in the liver) or metastatic (developed in another organ, then migrated to the liver). The majority of liver metastases come from the colon. The single tumor or more than one tumor confined to either left or right side of the liver can be successfully resected with 5-year survival as high as 60%.
Liver resection patients are carefully evaluated by a multidisciplinary team to ensure the absence of the extrahepatic (outside the liver) tumor. Liver resections performed on patients with extrahepatic disease may relieve the symptoms caused by the tumor, but offer little improvement in survival.
Benign tumors of the liver (cyst, adenoma, hemangioma) can be successfully managed by liver resection as well. If the location of a benign tumor is superficial and small in size, the operation can be performed laparoscopically (by making small punctures in the abdomen while viewing through a video camera).
Liver resections are also performed on people willing to donate part of their liver to a loved one (see live donor liver transplant).
A liver resection takes approximately 3-5 hours and can be performed without the need for blood transfusion (see bloodless surgery). Up to 75% of the liver tissue can be safely removed. The hospital stay is about 5 days and complete recovery occurs in 5-6 weeks. The resected liver regenerates to its preoperative size in 6-8 weeks. Excellent results from liver resections are usually achieved.
| LIVE DONOR LIVER TRANSPLANT |
Live donor liver transplantation (LDLT) is a procedure in which a living person donates a portion of his or her liver to another. The feasibility of LDLT was first demonstrated in the United States in 1989. The recipient was a child, who received a segment of his mother's liver. Since that time, LDLT for children has enjoyed wide success and many pediatric programs use this technique.
In the pediatric experience, survival of both the recipient and the transplanted liver (graft) at 1 year is about 90%. Donor complications have been very few. A rising population of adult patients awaiting liver transplantation has led to the application of LDLT for adult patients, and the preliminary results have been very encouraging. Only a handful of centers in this country perform the procedure.
|
PANCREATIC SURGERY
Pancreatic surgery encompasses a wide variety of surgical procedures concerning the pancreas (a gland located behind the stomach just below the liver). Disorders of pancreas can be divided onto those caused by tumors (benign or malignant) and those caused by inflammation (acute or chronic).
The majority of surgical procedures performed on the pancreas involve resection (removal) of the portion that is involved in the disease process. Prior to any operation on the pancreas the patient undergoes testing and is evaluated by multidisciplinary team of physicians. The management approaches to acute and chronic pancreatitis are different and may not necessarily involve surgical intervention. Often excellent results can be achieved through medical management.
A major pancreatic resection takes approximately 4-6 hours and in most cases is performed without blood transfusion (see bloodless surgery). The post-operative hospital stay is about 7 days and complete recuperation time is expected in 6 weeks. In properly selected patients, excellent operative results and future quality of life are achieved.
GALLBLADDER / BILE DUCT SURGERY
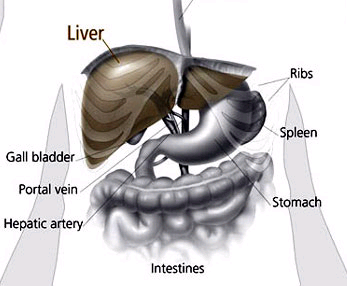
The bile duct system and gallbladder (collectively known as the biliary tree) are involved in the drainage and delivery of bile from the liver into the intestine. Bile production is one of the most vital functions of the liver and it is necessary for the appropriate absorption of nutrients from the intestine. Disorders of the biliary tree can alter this function. The gallbladder is located underneath the liver and the bile duct extends from inside the liver into the duodenum (initial portion of the small intestine just past the stomach). The bile duct has an extrahepatic portion (outside the liver) and intrapancreatic portion (within the pancreas).
The most common disorder of the biliary tree is cholelithiasis or gallstones. Gallstones are usually located in the gallbladder and, if symptomatic, can be removed laparoscopically (without open surgery) along with the gallbladder. There is a 1 to 2 day hospital stay after this operation and full recuperation time is about two weeks. The presence of gallstones can be complicated by acute pancreatitis (see pancreatic surgery).
The biliary tree can be a site for the growth of malignant tumors. In this case the removal of a portion of bile duct may be necessary. Depending on tumor location, complete removal of the tumor may also involve concomitant resection of the liver (see liver surgery) or pancreas (see pancreatic surgery).
Certain diseases of the biliary tree (i.e. primary sclerosing cholangitis) may also injure the liver and progress to end-stage liver disease. In such cases liver transplantation may be the only option (see liver transplantation).
Operations on the biliary tree can be done very safely and usually without blood transfusion (see bloodless surgery). If major resections of liver or pancreas are involved, the operative time is about 3-6 hours. The hospital stay is about 7 days and full recuperation time is about 6 weeks. Under most circumstances, excellent outcomes are usually achieved.
PORTAL HYPERTENSION SURGERY
The liver filters venous blood from abdominal organs. Portal hypertension is increased blood pressure in the veins of abdominal organs. The primary vein that carries blood from the abdominal organs to the liver is called the portal vein. When this vein clots or when the liver develops scar tissue from disease and compresses the vein, the blood pressure in the vein goes up and portal hypertension develops. Blood backing up in the veins of abdominal organs causes typical signs of portal hypertension such as ascites to develop. Ascites is free fluid in the abdomen caused by blood being under high pressure and some of its liquid portion squeezing through the vessels and settling in the abdomen.
Hypersplenism is an enlarged spleen caused by blood congestion and increased destruction of blood cells due to spleen hyperactivity. Gastrointestinal bleeding (bleeding into the stomach) results from rupture of varicose veins in the stomach and esophagus (swallowing tube). Varicose veins form a collateral venous network for the blood to escape into an area of lower pressure.
Portal hypertension can be accompanied by good liver function with good production of all necessary proteins. In such instances liver transplantation is not indicated (see liver transplantation). For long-term management an operation called portal vein shunting can be considered. During this operation the surgical connection between the portal vein or its branches and the vena cava (low-pressure vein caring blood from lower extremities and kidneys to the heart) or its branches is created. This allows blood from the portal vein to be redirected into the vena cava resolving the portal hypertension. This operation can be performed in selected patients with excellent long-term results.
RADIO FREQUENCY ABLATION
Radio-frequency is a type of electrical energy that has been used in medical procedures for decades. At the most basic level, this electrical energy is used to create heat. The heat is created in a specific location, at a specific temperature, for a specific period of time, and ultimately results in the death of unwanted tissue.
During a radio-frequency procedure, an ablation probe is placed directly into the target tissue. An array of several small, curved electrodes are deployed from the end of the probe into the tissue. The generator is turned on and target temperatures are input. The radio-frequency energy flows through the electrodes, causing ionic agitation, and therefore friction, in the nearby tissue. This friction creates heat, and once sufficient temperatures have been reached, the heat kills the target tissue within a few minutes. Thermocouples (tiny thermometers) incorporated into the tips of the electrodes allow continuous monitoring of tissue temperatures, and power is automatically adjusted so that the target temperatures remain constant. Ultrasound is typically used to monitor the treatment process.
Heat is a very effective means of killing tissue. As tissue temperature rises above 113° F (50° C), protein is permanently damaged and cell membranes fuse. The process is rapid, typically requiring less than 10-15 minutes exposure time for a 3 cm ablation.
Depending on the power applied and the resistance of the tissues, heat decreases rapidly at a specific distance from the electrode tip, limiting the ablation size. The size of the ablated area is determined largely by the size of the probe, the temperature of the tissue, and the duration of time the energy is applied. There is a sharp boundary between dead tissue and unaffected surrounding tissue. Thus unwanted tissue can be ablated without much sacrifice of surrounding normal tissue.
What is an RF Procedure Like?
Your physician can tell you what to expect before and after the procedure. There are several different ways that a RF procedure may be performed, and each has different benefits, limitations, and applicability. Your physician can determine which is most suitable for you.
One option is a percutaneous approach, in which the electrode is inserted through the skin to the desired location. The physician usually uses ultrasound to guide the needle to the right location. This is the least invasive way that RF is performed. General anesthesia is usually not necessary, but typically the patient is sedated. Often the patient is able to go home the same day.
If general anesthesia is not used, some discomfort or pain may be felt while the area is being ablated.
Options
Another option is a laparoscopic approach. With this approach, the surgeon makes a few small incisions in the abdomen, through which the necessary instruments are passed in order to treat the target tissue. This is also a minimally invasive approach, although general anesthesia is necessary. Patients typically go home the next day. One advantage of this approach is that intraoperative ultrasound can be used, which may result in more accurate location and visualization of the target tissue.
A third option is the open approach. This is what most people probably think of when they think of an operation. An incision is made in the area to be treated, and the surgeon can directly visualize the procedure. General anesthesia is necessary, and the recovery period is a bit longer.
Patients may experience a slight fever for two or three days after the procedure. Physicians often allow the fever to resolve without intervention.
RF ablation procedures have a relatively low rate of complications (~ 3.6%). Most of the complications are considered minor. The following are the complications associated with this procedure: infection (abscess), bleeding, collapse of the lung, abnormal heart rhythms, and skin burn.
ERCP
Endoscopic retrograde cholangiopancreatography (en-doh-SKAH-pik REH-troh-grayd koh-LAN-jee-oh-PANG-kree-uh-TAH-gruh-fee) (ERCP) enables the physician to diagnose problems in the liver, gallbladder, bile ducts, and pancreas. The liver is a large organ that, among other things, makes a liquid called bile that helps with digestion. The gallbladder is a small, pear-shaped organ that stores bile until it is needed for digestion. The bile ducts are tubes that carry bile from the liver to the gallbladder and small intestine. These ducts are sometimes called the biliary tree. The pancreas is a large gland that produces chemicals that help with digestion.
ERCP may be used to discover the reason for jaundice, upper abdominal pain, and unexplained weight loss. ERCP combines the use of x-rays and an endoscope, which is a long, flexible, lighted tube. Through it, the physician can see the inside of the stomach, duodenum, and ducts in the biliary tree and pancreas.
The Procedure
For the procedure, you will lie on your left side on an examining table in an x-ray room. You will be given medication to help numb the back of your throat and a sedative to help you relax during the exam. You will swallow the endoscope, and the physician will then guide the scope through your esophagus, stomach, and duodenum until it reaches the spot where the ducts of the biliary tree and pancreas open into the duodenum. At this time, you will be turned to lie flat on your stomach, and the physician will pass a small plastic tube through the scope. Through the tube, the physician will inject a dye into the ducts to make them show up clearly on x-rays. A radiographer will begin taking x-rays as soon as the dye is injected.
If the exam shows a gallstone or narrowing of the ducts, the physician can insert instruments into the scope to remove or work around the obstruction. Also, tissue samples (biopsy) can be taken for further testing.
Possible complications of ERCP include pancreatitis (inflammation of the pancreas), infection, bleeding, and perforation of the duodenum. However, such problems are uncommon. You may have tenderness or a lump where the sedative was injected, but that should go away in a few days or weeks.
ERCP takes 30 minutes to 2 hours. You may have some discomfort when the physician blows air into the duodenum and injects the dye into the ducts. However, the pain medicine and sedative should keep you from feeling too much discomfort. After the procedure, you will need to stay at the physician's office for 1 to 2 hours until the sedative wears off. The physician will make sure you do not have signs of complications before you leave. If any kind of treatment is done during ERCP, such as removing a gallstone, you may need to stay in the hospital overnight.
Preparation
Your stomach and duodenum must be empty for the procedure to be accurate and safe. You will not be able to eat or drink anything after midnight the night before the procedure, or for 6 to 8 hours beforehand, depending on the time of your procedure. Also, the physician will need to know whether you have any allergies, especially to iodine, which is in the dye. You must also arrange for someone to take you home--you will not be allowed to drive because of the sedatives. The physician may give you other special instructions.
MAGNETIC RESONANCE CHOLANGIOPANCREATOGRAPHY
Magnetic Resonance Cholangiopancreatography represents a relatively new development in MR technology that allows for rapid evaluation of the biliary tract, pancreatic duct and gallbladder without contrast material administration, instrumentation or radiation. To date, over 2000 MRCPs have been performed at the Medical College of Virginia Hospitals. Special imaging sequences that are heavily-T2-weighted are utilized to depict the biliary tract, pancreatic duct and gallbladder as high signal intensity or bright structures owing to the fluid within them. Studies performed at the Medical College of Virginia Hospitals as well as at other institutions have shown that the accuracy of MRCP is comparable to that known as ERCP (endoscopic retrograde cholangiopancreatography, the traditional but invasive means of imaging the pancreaticobiliary system) in the evaluation of choledocholithiasis, malignant obstruction, anatomic variants and chronic pancreatitis. In most instances, MRCP can be completed in 10 minutes and is easily performed as an outpatient examination.
Since its introduction in 1991, the role of MRCP in evaluating pancreaticobiliary disease has continued to evolve. MRCP is assuming a larger role as a rapid, accurate and non-invasive alternative to diagnostic ERCP. During the past several years, radiologists and nonradiologists alike have shown a keen interest in MRCP and its clinical applications. Technical refinements such as fast MR sequences that allow for imaging of the entire biliary tract and pancreatic duct in a single breathhold have resulted in marked improvement in the quality and diagnostic yield of MRCPs. As the quality of MRCPs has improved, the clinical applications of this technique have expanded such that MRCP is now replacing diagnostic ERCP in many instances.
Current techniques allow for depiction of obstructed or dilated bile and pancreatic ducts in essentially all patients. Normal caliber extrahepatic bile ducts and central intrahepatic ducts are routinely depicted in as many as 100% of patients. Although the normal caliber pancreatic duct may be more difficult to visualize than the bile duct, the normal pancreatic duct can be visualized in 80-95% of cases. Dilated ducts proximal to an obstruction are well visualized, usually better than with ERCP where there can be difficulty in opacifying ducts proximal to a high-grade obstruction.
MRCP avoids the complications of ERCP such as pancreatitis (3-5%), sepsis, perforation and hemorrhage. The main disadvantage of MRCP is that it is purely diagnostic and does not provide access for therapeutic intervention.
MEET THE HEAD MASTER SURGEON

About
Dr.Subash Gupta, MBBS, MS, FRCS(Glas), FRCSEd.
Dr. Subash Gupta is a highly experienced liver surgeon with experience of over 400 hepatectomies and over 120 liver transplant operations both in England and in India. He started the liver transplant program at Sir Ganga Ram Hospital.
He has been associated with some of the best liver surgeons of this century starting from Paul McMaster of Queen Elizabeth University Hospital, Birmingham, Peter Lodge of St. James's University, Leeds, Leslie Blumgart from Memorial Sloan Kettering Hospital, New York, SG Lee of Asan Medical Centre, Seoul, Tanaka from Kyoto University and ST Fan of Queen Mary Hospital, Hong Kong.
He has incorporated the best points of these master surgeons to evolve a form of liver surgery that is fast, bloodless and least traumatic to the patient. He has transformed what was previously in India, a bloody and difficult operation to a safe and bloodless operation. He is frequently sought after to conduct hepatobiliary workshops all over India.
The one he conducted in Guwahati last September was attended by over 400 surgeons. The Gyan Burman Liver Unit attracts visitors and fellows for training throughout the year.
Dr. Subash Gupta schooled in St. Vincent’s School, Asansol and then began medical schooling in the prestigious All India Institute of Medical Sciences (AIIMS). After an excellent performance as a medical student, the department of surgery in AIIMS reinforced his inclination towards surgical sciences.
In the year 2003, the Gyan Burman Liver Surgery Unit was set up and this unit also trains experienced surgeons in advanced hepatobiliary surgery.
Dr. Gupta and his colleagues have performed many liver transplant operations in Sir Ganga Ram Hospital including:
- Cadaveric reduced liver transplantation in a child
- Right lobe adult to adult liver transplantation
- Left lobe adult to adult liver transplantation
- Combined liver kidney transplant operations
- Liver transplantation for hepatocellular carcinoma